WHAT IS PSORIASIS?
Psoriasis is a common, chronic, scaly rash that affects people of all ages (about 2% of the population). There is a genetic predisposition to psoriasis i.e. it tends to run in families.
Psoriasis is also influenced by many environmental factors. It is not contagious and is not due to an allergy.
The most common ages for psoriasis to first appear are in the late teens and in the 50s. It affects men and women equally, although in children, girls are more commonly affected than boys.
Psoriasis is often so mild it is barely noticed by the affected person, but it can occasionally be so severe the patient must be admitted to hospital for treatment. It may or may not be itchy.
What does psoriasis look like?
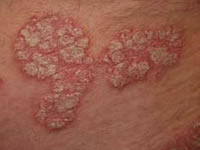
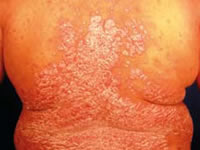
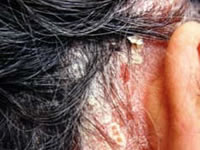
Psoriasis is characterised by red, scaly patches of skin, which usually have very well defined edges. It is often symmetrical, affecting both sides of the body. The scale is typically silvery white. This typical scale may not be so obvious if the psoriasis affects a body fold such as the armpit or the patient is using emollients regularly. Then it is more likely to be smooth and shiny.
Psoriasis is often very minor, causing a few dry patches on the backs of the elbows and knees, some irritation in the umbilicus (belly button) and natal cleft (between the buttocks) or scaling in the scalp. It can, however, affect any area of skin and it may be severe or unusual in appearance.
What causes psoriasis?
Exactly what causes psoriasis is not fully understood but there is a lot of active research into this area. The immune system is involved and appears to be overactive in a way that causes inflammation. Specifically, there is excessive production of cell growth compounds. These have many effects, including growth of extra blood vessels within the skin (causing the red colour) and increased turnover of the skin cells (causing the scaling and thickening of the skin).
Genetic influences
Like many diseases, psoriasis is influenced by inherited characteristics. Up to 50% of people with psoriasis will know of another affected family member. Patients with a family history of psoriasis tend to develop psoriasis earlier in life than those without a family history.
Stress
Physical and emotional stress may precipitate psoriasis and are hard to avoid.
Infection
Infections may cause flares of psoriasis. Sometimes, treatment of the infection may result in clearing or improvement of the psoriasis.
Streptococcal throat infections (tonsillitis) may cause guttate psoriasis.
Candida infections (thrush) may aggravate flexural psoriasis.
Malassezia yeasts may have a role in sebopsoriasis.
Injury
Psoriasis localises around the site of physical, chemical, electrical, infective and inflammatory injury as it heals (the Koebner phenomenon). Less often, psoriasis may localise to old scars.
Hormones
The relationship of hormones to psoriasis is unclear. Post-puberty is a peak time for the onset of psoriasis. Pregnancy may also have an effect on the severity of the psoriasis; it usually improves with the potential for worsening after the birth of the baby, but the reverse can occur.
Psoriasis does not affect the unborn baby.
Medications
Several medications can precipitate or aggravate psoriasis:
- Lithium
- Beta blockers (used to treat high blood pressure)
- Anti-malarials e.g. hydroxychloroquine
- Nonsteroidal anti-inflammatory drugs (NSA IDs)
- Stopping oral corticosteroids
- Stopping strong topical corticosteroids.
Sun and UV Light
- Ultraviolet light can precipitate or aggravate psoriasis.
- Sunlight is usually beneficial for psoriasis (except in sun sensitive / photosensitive psoriasis).
Obesity
Many psoriasis studies have noted many affected patients to be overweight or obese. Recently, it has become clear that the severity of psoriasis is correlated with insulin resistance, a feature of metabolic syndrome. Psoriasis is associated with a greater risk of atherosclerosis resulting in ischaemic heart disease (angina and heart attack), stroke and peripheral vascular disease.
Alcohol and smoking
There is an association between increased alcohol intake and smoking and the development of severe psoriasis. However, whether this is a cause, or effect, is not known.
Is there a cure?
There is to date no cure for psoriasis but satisfactory control of the disease is possible for most patients.
Some people have a single episode of psoriasis that clears after a few months and never recurs, quite likely after acute guttate psoriasis. Most other forms of psoriasis run a fluctuating course with periods of marked improvement and even complete clearance, only to relapse at a later time. There may be several years between relapses. A small group of patients have severe, persistent psoriasis that is very difficult to treat and can be very disabling.
1. Topical therapies
Treatments that are applied directly to the skin are known as topical therapies. They include creams, ointments, pastes and lotions. If your psoriasis is mild, topical therapies will be the mainstay of your treatment and include the following:
Emollients. Emollients reduce scaling and can be used as often as needed.
Salicylic acid. Preparations containing salicylic acid can help heavily scaled plaques.
Topical steroids. Weaker steroids often do not work very well on thick patches of psoriasis, but may do better on the face or in the skin folds. The stronger ones have possible side effects, one of which is to make your skin thinner. Your doctor will monitor their use closely. Psoriasis sometimes comes back quickly when topical steroid treatment stops.
Tar preparations. Taking a medicated tar bath may help to remove loose scales. Tar creams or ointments help most patients but may be messy and can stain clothing.
Vitamin D analogues. There are vitamin D preparations used to treat psoriasis. These are safe, clean to use and do not stain the skin. Treatment is applied twice daily and can go on for as long as required. Irritation may occur, especially on the face, buttocks and genitals, and these treatments should be applied to those areas only on the specific instructions of your doctor.
2. Phototherapy
This term refers to treatment with various forms of ultraviolet light, sometimes assisted by taking particular tablets. It is helpful if the psoriasis is extensive, or fails to clear with topical treatment, or comes back quickly after seeming to clear. Topical therapy will usually continue during the phototherapy.
Two types of ultraviolet (UV) light may be given, using special machines: UVA and UVB. These are different parts of normal sunlight. Treatment with UVA is helped by taking a medication known as a psoralen – a combination known as PUVA therapy. Treatment with UVB does not need tablets.
3. Oral and Injected Treatments
The idea of using a tablet to treat psoriasis is attractive, but the effective ones all have potential risks, so they are not used for psoriasis if it can be kept under control in simpler ways. In addition, you will usually have to continue with some topical therapy even though you are taking the tablets.
Your dermatologist will discuss the risks with you if you start on this kind of treatment. All of the tablets may require blood tests, and many interfere with other medicines. Female patients should not become pregnant whilst on any tablets for psoriasis, and with some of them it is important that male patients should not father a child.
Other than Novatretin, the tablets in question include ciclosporin (suppresses the immune system), methotrexate (slows down the rate at which the skin cells are dividing in psoriasis), and hydroxycarbamide (formerly known as hydroxyurea – also slows down the rate at which the skin cells are dividing).
There are also several injectable forms of treatment known as “Biologicals” available for extremely severe forms of psoriasis.
Psoriasis of the palms and soles
Psoriasis may predominantly affect the palms and soles in various ways:
- Typical scaly, red patches similar to psoriasis elsewhere
- Generalised thickening and scaling of the palms and soles (keratoderma)
- Sheets of tiny yellow-brown pustules (palmoplantar pustulosis).
Palmoplantar psoriasis
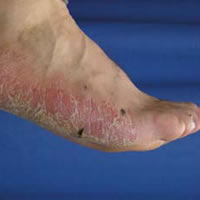
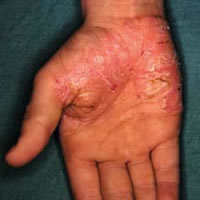
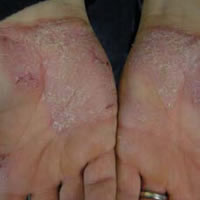
Clinical features
Palms and soles affected by psoriasis tend to be partially or completely red, dry and thickened, often with deep painful cracks (fissures). It can be quite hard to differentiate from hand dermatitis and other forms of keratoderma, but signs of psoriasis elsewhere may help make a diagnosis.
Palmoplantar pustulosis is considered a distinct entity in which there are clusters of pustules on the palms and/or soles, but about 10-20% of those affected have psoriasis on other sites of the body.
Palmoplantar psoriasis tends to be a chronic recurrent condition.
Treatment
Mild psoriasis of the palms and soles may be treated with topical treatments:
- Emollients: thick, greasy barrier creams applied thinly and frequently to moisturise the dry, scaly skin and help prevent painful cracking.
- Keratolytic agents such as urea or salicylic acid to thin down thick scaling skin. Several companies market effective heel balms containing these agents.
- Coal tar: to improve the scale and inflammation. Because of the mess, coal tar is often applied at night under cotton gloves.
- Topical steroids: ultrapotent ointment applied initially daily for two to four weeks, if necessary under occlusion, to reduce inflammation, itch and scaling. Maintenance use should be confined to 2 days each week (weekend pulses) to avoid thinning the skin and causing the psoriasis to become more extensive.
Calcipotriol ointment is not very successful for palmoplantar psoriasis and may cause an irritant dermatitis on the face if a treated area inadvertently touches it. Dithranol is too messy for routine use on hands and feet.
More severe palmoplantar psoriasis usually requires phototherapy or systemic agents, most often:
- PUVA
- Acitretin
- Methotrexate
Biologics are also sometimes prescribed for severe palmoplantar psoriasis.