TREATING DARIER’S DISEASE
Darier disease is also known as ‘keratosis follicularis’. It is a genetic disorder that causes skin changes. Onset of skin changes is usually in adolescence and the disease is usually long term. It is inherited in an autosomal dominant pattern, which means that a single gene passed from one parent causes the condition. The chance of a child inheriting the abnormal gene if one parent is affected is 1 in 2 (50%) but not all people with the abnormal gene will develop symptoms of the disease.
How is it diagnosed ?
Usually Darier disease is diagnosed by its appearance and the family history, but it is often mistaken for other skin problems.
The symptoms and signs of Darier disease vary between individuals. Some have very subtle signs that are found only on careful inspection. Others have extensive lesions. In an affected person the severity of the disease can fluctuate over time.
Skin rash
The skin lesions are greasy, scaly papules (small bumps) which tend to occur over the oily areas of the face (scalp margins, forehead, ears, around the nostrils and sides of nose, eyebrows, and beard area), neck, and central chest and back. The flexures (within natural folds of the skin around joints such as armpits and groins) and skin under breasts and between buttocks are also commonly affected. The papules have a firm, harsh feel like coarse sandpaper and may be skincoloured, yellow-brown or brown in colour. If several of the small papules grow together they may form larger warty lesions which can become quite smelly within skin folds. The scalp is often affected with a heavily crusted rash which can be similar to seborrhoeic dermatitis but is usually harsher to the touch.
Other presentations of this disease are common. Some patients may have flat, freckle-like lesions. Others may have very large, raised, warty lesions. Cystic acne may occur.
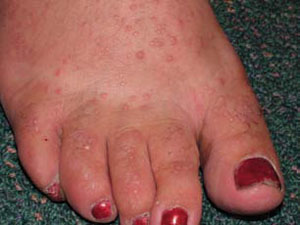
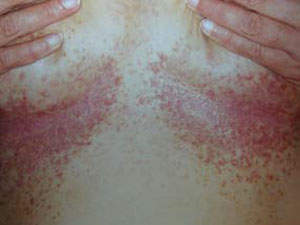
Lesions affecting the mucous membranes
Mucous membranes are the red, moist linings of all body surfaces except the skin (eg. mouth, oesophagus, rectum, vulva, vagina). Patients with Darier disease may uncommonly have a white cobblestone pattern or small papules affecting the mucous membranes. Overgrowth of the gums is also seen.
Most patients will develop signs of the disease (even if subtle) before the age of 30 years. Many patients will have a mild form of the disease that, although present, will go unnoticed throughout life. Patients with more severe disease will notice a chronic relapsing-remitting pattern to their signs and symptoms although cases of spontaneous resolution of signs have been reported. The rash is often exacerbated by sunlight (a reaction which may be delayed eg. on return from holiday), and occasionally by steroid use (although this may be useful for other
patients). Bacterial infection can cause flares. Widespread infection of the skin with the herpes simplex (coldsore) virus is a well recognised complication. This can cause a severe flare and patients can feel quite unwell.
In most patients general health remains good regardless of the severity of the disease.
Treatment
Treatment is required only if there are troublesome symptoms. For patients with mild disease simple moisturisers, sun protection and selection of the right clothing to avoid heat and sweating are usually sufficient.
Dermabrasion (sanding off the surface of the skin) may be effective in localised disease.
Localised Darier disease may also be treated successfully with topical retinoids. Secondary bacterial infection (usually due to Staphylococcus aureus) should be treated with antibiotics, and herpes simplex with antiviral agents.
If symptoms are particularly severe then a trial of an oral retinoid medication such as acitretin may be effective.